"An incredible South African community hospital"
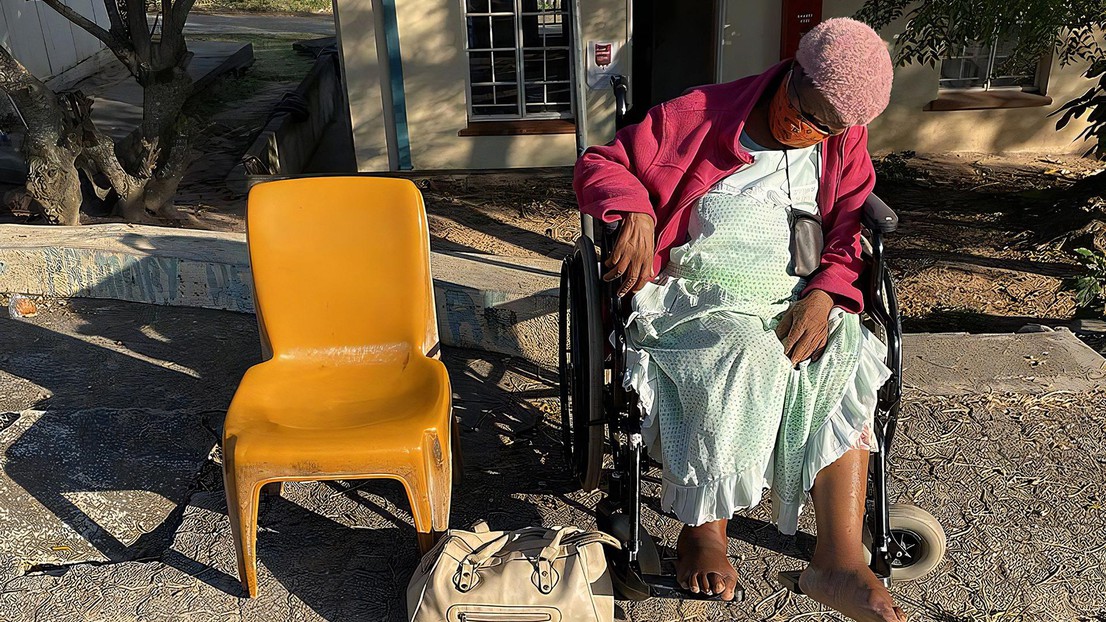
Critically ill patient waiting for emergency room care © 2021 Mary Anne Hartley / EPFL
EPFL’s Dr Mary-Anne Hartley is currently volunteering as a medical doctor in a rural hospital in South Africa. Surrounded by bush and wildlife, it seems a long way from her work using the latest technologies in artificial intelligence to identify patterns of COVID in lung images, but that is exactly what she went there to do.
Rural medicine is an unpredictable and exciting mix of disciplines, limitations and absurdities that requires flexibility, creativity and good humour to make it through an "average" day as a doctor. And this is no more so than in an under-resourced, remote hospital in the South African province of Mpumalanga, not far from the Kruger National Park and the country’s border with Mozambique.
For the past month, a small hut in a nature reserve near Tintswalo Hospital has been home to EPFL’s Dr Mary Anne Hartley, Head of Intelligent Global Health (iGH), hosted at the Machine Learning and Optimization Laboratory (MLO), part of the School of Computer and Communication Sciences.
Staffed by highly dedicated and competent health workers, the hospital is the only option for half a million people in the catchment area, treating about 4000 patients a month. It also supports about 50 surrounding clinics and provides services ranging from eyeglasses to amputations.
Her daily commute can be quite something. “Sometimes I find grouchy elephants on my doorstep and have to compete with warthog traffic jams to make it to work on time. Closer to the hospital, it’s a game of dodging massive potholes, rogue poultry, the occasional riot and a distressing number of stray dogs,” Hartley says.
There have been some close calls too, “I recently stepped on what I thought to be a very unimpressive looking snake. It was only about 50cm long and barely thicker than a thumb, so I gently shooed it off the path with a stick. Taking exception to being moved, it puffed up its orange neck, which identified it as a Twig Snake, one of the most hemotoxic snakes on the planet... and without any antivenom. Lesson learned - size doesn’t matter!”

In addition to setting up her research study on artificially intelligent lung imaging, as in any other hospital, Hartley mostly sees patients with cancers, heart failure and strokes, but here, they are almost always complicated by a complex cocktail of tropical and frustratingly preventable diseases like HIV, and TB. Some days she may help at one of the surrounding clinics, run by a skeleton crew of dedicated nursing staff, who request a medical doctor for the day to deal with their more complex patients unable to attend the hospital. “It’s a bumpy drive over dirt roads to an outpost where the queue is longer than the perimeter of the clinic,” she explains.
The hospital building was originally constructed by missionaries during the apartheid era and is surrounded by dense rural shanty towns that have no running water or electricity. The emergency room is little more than a rundown hole in the wall where a destroyed door hangs off a hinge and almost everything is broken. During rains, the roof leaks asbestos-tainted water directly onto patients and rotted layers of vinyl make up the floor, which is impossible to clean.
A common theme is making do - fixing semi-functional equipment or improvising alternatives for missing stock. Each day, patients sit outside in the gutter in the blazing sun and brace themselves for an 8-hour day of waiting to be seen. Fried chicken feet are sold through the fence to those who can afford it.
But for Hartley, most shockingly, the hospital has no triage system in place, “This is the fundamental and life-saving assessment that prioritizes patients into colour-coded severity categories - green, yellow, orange, red, and it’s simply because there is no infrastructure. It is not uncommon for a patient to die directly because they deteriorated waiting all day in the sun behind a queue of less severe patients. This happened to me, and I snapped.”
She launched a fundraiser for urgent renovations to enable the implementation of a triage system, as well as a major structural re-organization to ensure streamlined care - both will save lives and make a major difference to health outcomes.
Hartley’s key inspiration comes from the hospital’s patients whom she is always surprised to find polite and thankful for the service they get, despite the appalling conditions. It’s a community, she says, with a rich heritage and a resilience only made possible from a lifetime of disappointment and crippling poverty.
“It is deeply frustrating working here. At the same time, however, I value the frustration as it forces creativity. It is why I love volunteering here. I enjoy finding challenges and the satisfaction of resolving them.”
Dr Hartley has so far raised donations that have fixed the floor, installed curtains and some basic elements of the triage, but her and the team are seeking more for the roof, mattresses, and life-saving equipment such as suction and monitors.